IGENEX TICK-BORNE
DISEASE TESTING
Note: This is not an at-home test. You still need a doctor’s authorization, and you will send your sample back to IGeneX for testing.
CHOOSE A
COLLECTION KIT
BLOOD COLLECTION KIT
URINE COLLECTION KIT
MISC. COLLECTION KIT
HOW IT WORKS


Order a kit
Order a collection kit right here on the IGeneX website for a small deposit that will be applied to your testing fees.
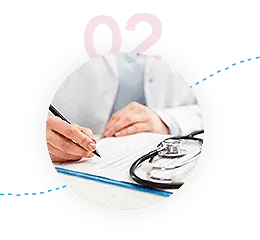

Complete Paperwork
Complete the paperwork with your doctor to determine which tests IGeneX should conduct with your samples.
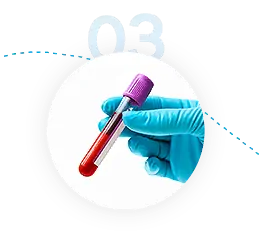


Get Results
Ship everything to IGeneX. We will conduct the appropriate tests and send the results to your doctor in 7-10 business days..
HEAR FROM OUR PATIENTS
"IGeneX is so worth the money..."
YouTuber Carly Melissa used IGeneX tests to confirm her diagnosis of Lyme disease and a coinfection of Bartonellosis (Cat Scratch Disease). Hear her discuss her Lyme journey, from a bull’s eye rash she didn’t recognize to her upcoming antibiotic treatment.
"IGeneX is the only reliable test."
"My best bet was to use IGeneX."
Meghan Bradshaw had to give up her career in retail due to a tick-borne illness. Hear her discuss how testing with IGeneX helped her get the proper diagnosis.
RESULTS YOU CAN UNDERSTAND

Gain meaningful insights about your health with easy-to-understand test results. We also provide you with additional resources and helpful tips along the way.

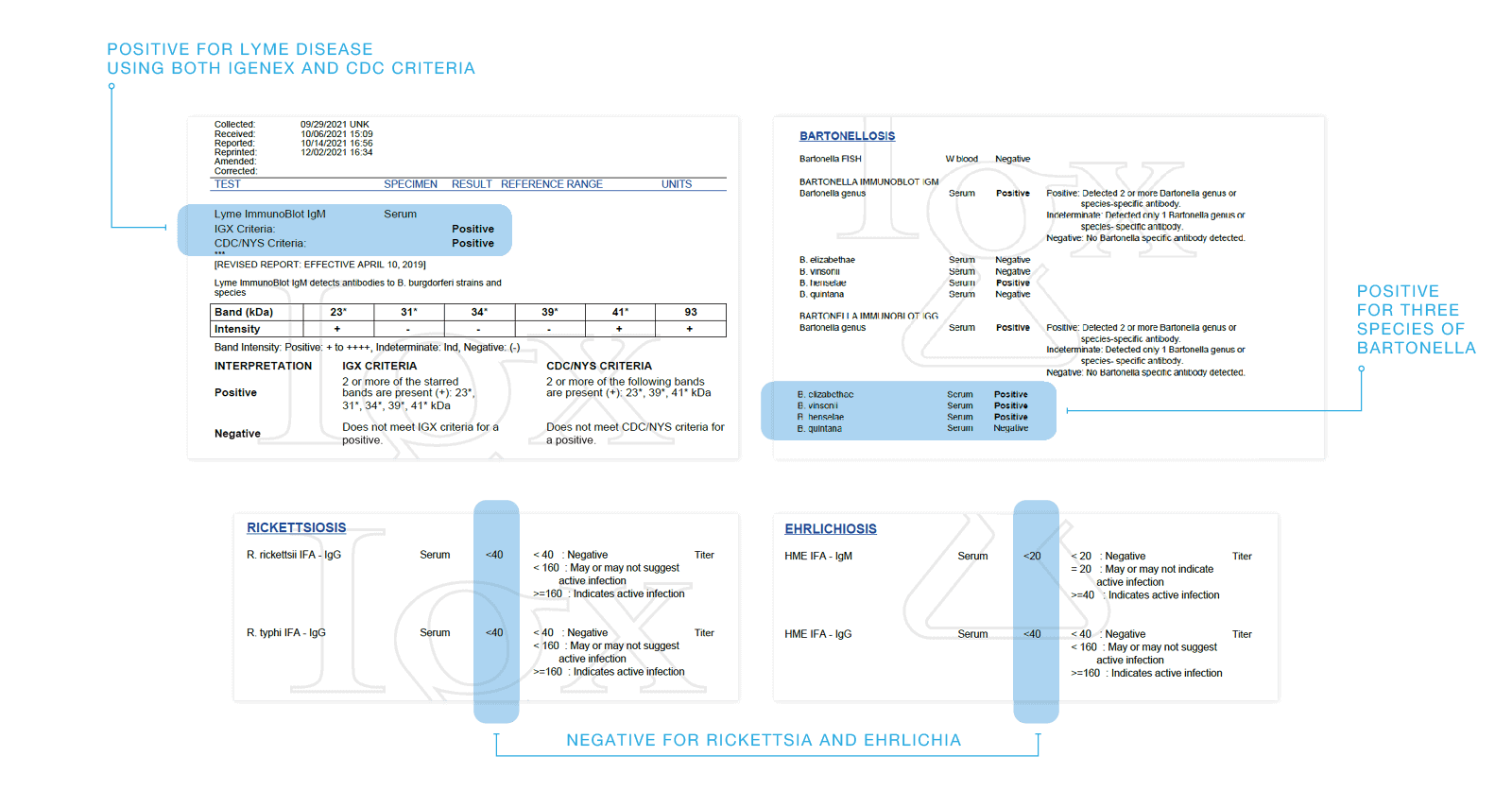
Get detailed information on the results of your tests, including information comparing your results based on IGeneX and CDC criteria.

Take action on your health and wellness. Use your report to help guide your next steps. Contact your healthcare provider to learn more about your results and get your questions answered.

Gain meaningful insights about your health with easy-to-understand test results. We also provide you with additional resources and helpful tips along the way.

Get detailed information on the results of your tests, including information comparing your results based on IGeneX and CDC criteria.

Take action on your health and wellness. Use your report to help guide your next steps. Contact your healthcare provider to learn more about your results and get your questions answered.
WHY IGENEX FOR TICK-BORNE DISEASE TESTING?

- CLIA certified in all 50 states
- Long track record of success since 1991
- Offers testing that is nearly twice as accurate as CDC recommended tests
- Tests for all major tick-borne illnesses, including Lyme disease, TBRF, Babesia, Bartonella, and Rickettsia
- Utilizes comprehensive testing methods such as PCR, ImmunoBlots, IgXSpot and FISH
- Has become a nationwide leader in COVID-19 testing due to a relentless focus on customer satisfaction
Test a Tick
If you are bitten by a tick and are able to remove it and send it in, or if you find one and aren’t sure if you’ve been bit, IGeneX can test the tick to determine if it is carrying the pathogens that can lead to tick-borne illnesses. Go here to learn more.






My first Lyme test with my primary care doctor did not show a positive, but my symptoms persisted for another six months. I did some herbal therapy which helped ease the aches and nausea, but I still did not feel great and felt I need another test. I chose to get tested at IGeneX after talking with a Lyme literate doctor. The test showed positive for Lyme. It was expensive, but I think worth it ultimately.